Improvement science may be defined as the study of the cumulative effectiveness of system change under bounded Predictability[Uncertainty and Complexity]. It is my contention that the various components of this definition are sufficient to characterize the essence of the field. However each of these terms needs elaboration to include necessary assumptions.
In general terms, the uncertainty of the context may arise due to one or more of the following causes: a] dynamic nature of clinical work. It could be people centered, changing, and prone to disequilibrium. b] variation in the structures, processes and outcomes, with weak standardization c] complexity due to multi variate factors , due to multiplicity of personnel and decision making , lack of consensus , ubiquitous tradeoffs , multiplicity of conditions i.e. co morbidities , multiplicity of interventions applied either in parallel or in series. D] Uncontrolled due to long feedback loops, weak coupling of activities, dispersion of problem solving space e] culture dependent to differences in preferences, knowledge bases and resources. In its 1999 report on medical errors, To Err Is Human, the Institute of Medicine (IOM) notes that health care differs from a systematic production process “mostly because of huge variability in patients and circumstances, the need to adapt processes quickly, the rapidly changing knowledge base, and the importance of highly trained professionals who must use expert judgment in dynamic settings.”
Similarly, the assumptions about change are all multidimensional a] systemic b] collaborative c] continuous d] creative. The source of the change is a combination of evidence, best practice and convenience. There are generalizable expectations about the new system too. That there is a reduction in complexity i.e. simplification, Simplification: Maximizing Effect; Minimizing Effort that the new system is sustainable and most importantly that it is significant or meaningful depending on the dimension that serves as the objective of the change i.e. clinical outcomes, safety, satisfaction or cost etc.
The overall logic of improvement science is that there is a causal intervention on the system and the reaction or outcome is a new system. Its distinguishing feature is that it s new i.e. there is a break from the past that is deliberate. The intervention becomes causal as it is based on the knowledge of the system. The validity of the change is based on its consequence and is measured in terms of the chance of the success. It is more or less agreed by most of the scholars in the field that all factors that could be causally correlated with successful outcome are contained in Deming’s characterization of the theory of profound knowledge.
Irrespective of what is the case or system under test, we could elaborate individual contextually relevant factors that would reasonably and comprehensively define the success. In other words the answer to the question: what could you do to increase the chance of success? Better understanding of the causal intervention- what ever it may be , the desired outcome or goal are essentially based on knowledge , the nature of that knowledge and the limits of that knowledge , all of which are traditionally the concern of epistemology. In the clinical context it could be generisable scientific evidence. The use of the systematic method, the objective cognition of interdependencies, the role of technology, communication etc constitutes systems thinking. The evidence base, monitoring or evaluation and the dependence on measurement and data is related to statistical thinking. Participation of the right people, the exploitation of expertise and experience, better people and incentives require psychology.
The epistemic confidence that qualifies improvement with the above features as a science is its ability to predict within limits, over short time spans, through a process of model based or abductive reasoning. The goal is a conjecture that is the aim of the system derived from outliers in the practice pattern, the expectation of users or the capability of the domain ie. the evidence base.
The guarantee of success is the pragmatic application of prioritization, the multiplicity of the intervention and the cumulative progress due to its recursive application of its method and its persistence in the face of failure. These are the very factors that enable experiential learning as well as its synergistic effect of the casually correlated intervention. That the justification for the change is based on consensus is not necessary. Its sufficiency is derived from the fact that it is tested or actively justified by the consequences or usefulness. Thus the knowledge is actively justified effect or its cash value. It is the nature of the new system that lends validity to the change .The specific intervention whether drug or decision is identified backward reasoning from the aim or goal. That is never a crude maximum but a knowledge based optimum.
The concept of collaboration or collectiveness, the scope of intervention, whether focal or system-wide and dimensions that motivate the intervention i.e. Efficiency, cost, speed. They are the result of system thinking not prerequisite for change and not inseparable from the method as historically demonstrated by the case of QC adoption by American companies in the sixties. It is mark of versatility of the method that it accommodates group decision making. Collectivity and consensus have no justificatory role, but merely enhance the efficiency of the method. Thus are meta-systemic issues, just as standards or procedures.
Change is not improvement. Improvement is effective change. Improvement science is knowledge of the dynamics of change in a dynamic, real place, real time context. The effectiveness of change includes its significance, reproducibility and predictability. The significance of change is embodied in the dimension of quality and is value based in its varied formulations. The validity of change depends both on its precursors i.e. evidence or possibility of benefit as well as the objective change-effect relationship of its method. It is a statement of the causal modal underlying the change. The complex relationship between input, action and output. The predictability of the change is the expression of the statistical control of critical process related factors .It is merely the measure of the temporal consistency of the process that is undergoing transformation .This is a temporal description of change within desired functional limits . Reproducibility is the decontextualising principle that permits adaption, spread and verification in different contexts. All four of these characteristics are determinants of the chance of success of the change. While significance and reproducibility are at the systemic level, validity and reproducibility are at the process level. The former is derived from systems thinking and the latter from statistical thinking.
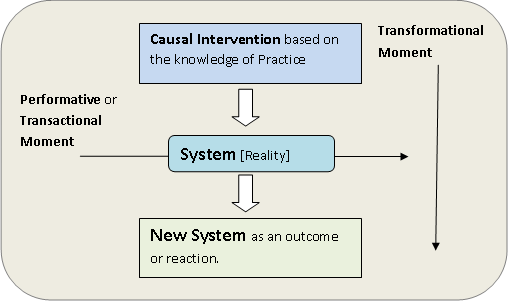
Evidence, Standard, speed, spread are extrinsic criteria and thus not necessarily or definitive of improvement science.
Viewing improvement as a technology is a view that is implicit in the particular approach called implementation science .Where it is seen as an applied extension of evidence based medicine or information mastery techniques. This however is an underestimation, as it denies the possibility of the fundamental nature of medical nature and practice. A view that is more present in the work of Brent James, Donald Berwick and Paul Batalden. A rebellion against the modern characterization of medical science merely as the application of other sciences – commonly called as basic sciences. In this schema, the study of practice is optional or contingent. Improvement science denies the gap between research and evaluation.
In a different emphasis Blumenthal, Bataden raise definitional issues in the over emphasis on systems or more specifically the exclusion of the professional. This once again is a different emphasis on practice as professionalism is the relationship between the individual and work.
The ideal of continuous improvement is susceptible a infinite regress. if change is all pervading , then the change also implies to the methods of change and they to further change of methods , thus leading to a never-ending regress. This regress can only be stemmed by greater clarification of the objective of change: balance the voice of the process with the voice of the customer.
The aggregate in medicine is not macro but merely epidemiological. But how is the claims to epidemiological effectiveness validated.
Effectiveness is both clinical [patient] and epidemiological [population]. Micro and Macro.
Focus on the small science
Nature of Actionable Data
0